- Revenue Cycle Management
- COVID-19
- Reimbursement
- Diabetes Awareness Month
- Risk Management
- Patient Retention
- Staffing
- Medical Economics® 100th Anniversary
- Coding and documentation
- Business of Endocrinology
- Telehealth
- Physicians Financial News
- Cybersecurity
- Cardiovascular Clinical Consult
- Locum Tenens, brought to you by LocumLife®
- Weight Management
- Business of Women's Health
- Practice Efficiency
- Finance and Wealth
- EHRs
- Remote Patient Monitoring
- Sponsored Webinars
- Medical Technology
- Billing and collections
- Acute Pain Management
- Exclusive Content
- Value-based Care
- Business of Pediatrics
- Concierge Medicine 2.0 by Castle Connolly Private Health Partners
- Practice Growth
- Concierge Medicine
- Business of Cardiology
- Implementing the Topcon Ocular Telehealth Platform
- Malpractice
- Influenza
- Sexual Health
- Chronic Conditions
- Technology
- Legal and Policy
- Money
- Opinion
- Vaccines
- Practice Management
- Patient Relations
- Careers
Practice Beat
Payer Contracts, Access to Care, Physician Shortages, Regulatory Reform, Medicaid
Practice Beat
Joan R. Rose
Payer Contracts: Doctors in the Garden State may flex bigger muscles
Noting that physicians lack sufficient market power to reject unfair contract terms that impede their ability to deliver medically appropriate care, New Jersey legislatorslike their counter- parts in Texas and Washington statehave decided to level the playing field. Under a measure signed into law on Jan. 8, two or more independent physicians can choose a representative to negotiate jointly with the carrier on their behalf.
While the bill focuses primarily on non-fee-related issues, doctors can enter into fee negotiations if the state attorney general determines a carrier's market power to pose a threat to the quality of patient care.
Although participation by the carrier will be voluntary, the state medical society terms the measure a good "starting point."
Regulatory Reform: A move to ease physicians' hassles with Medicare
Physicians who are audited and found to have been overpaid by Medicare would find it easier to make repayment if the Senate approves the Medicare Regulatory and Contracting Reform Act of 2001. If a lump-sum repayment would be a hardship on the physician, carriers would have to offer an installment plan instead of setting a 30-day deadline. Moreover, contractors generally couldn't use just a small number of claims to calculate overall amounts owed. And while they'd still be able to conduct random prepayment reviews, they would be prohibited from targeting a doctor for such review without cause.
Access to care: HHS' newest safety net: vending machines
Community health centers and other "safety net" organizations currently purchase most drugs at discounts of 25 to 40 percent. But their patients often can't afford to travel to distant pharmacies. Now HHS has approved a novel demonstration project to dispense prescription drugs through vending machines at remote health clinics.
Health care providers at the clinics will fax prescription orders to the Community Health Association of Spokane. Pharmacists there will fill the order via computer link to a locked vending machine at one of four networked clinics. A pharmacy technician will pick up the dispensed medication, attach a label, and deliver it to the waiting patient.
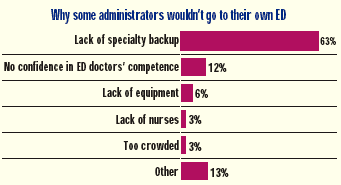
Physician Shortages: How the dwindling number of medical specialists is hurting ED care
Last year, more than a third of hospital emergency departments were forced to divert patients because of overcrowding, according to ED and hospital administrators polled by The Schumacher Group, a physician staffing organization. The survey suggests that a shortage of medical specialists is even more troubling for hospitalsand ED patients.
Two out of three hospitals transferred or diverted ED patients because they lacked specialty coverage. Three out of five respondents reported diverting ED patients for this reason at least three times a month, while one in three does so six or more times a month. And while the majority of administrators believe they have adequate specialty coverage for their EDs, 16 percent (up from 11 percent in 2000) said they would go to another hospital if they needed emergency care.
Medicaid: The Volunteer State appreciates its doctors in a big way
Christmas came early for a group of Tennessee physicians who participated in the state's program for Medicaid beneficiaries and the uninsured. In mid-December, the state mailed out checks totaling $25 million to doctors who treat a disproportionate share of TennCare enrollees. About 3,000 physicians (a third of those who participate in the program) shared in the largess. Payments were based on services billed in 2000 and could not exceed $50,000.
The governor had promised to reward the physicians who provide 70 percent of the care received by the program's enrollees and included the sum in his fiscal 2002 budget.
The author is a Contributing Writer.
Joan Rose. Practice Beat. Medical Economics 2002;4:15.
