Article
You can negotiate with health plans
Author(s):
Bargaining with powerful insurers may be harder than ever, but that doesn't mean you should accept their fees hands down.

Key Points
The first lesson about negotiations with health insurers is this: Don't throw in the towel before the fight even starts. Granted, it's understandable that doctors, especially those in small practices, feel hopeless and helpless about their ability to bargain with giant health plans for better pay. Due to insurance industry consolidation, the plans are getting even bigger and enjoying less competition. So it's easier for them to dictate contract terms, says Virginia Beach, VA, practice management consultant Greg Mertz.
"I've seen more insurance company stonewalling in the last two years than in my entire career," says Mertz. "It's David vs Goliath, but David is getting stepped on."
However, you may have more bargaining power than you think. Depending on your location, your specialty, and the size of your practice, insurers may actually want to keep you happy, especially if you threaten to walk away from a bad deal. If nothing else, negotiations may reveal that lowball reimbursement for a particular code is nothing more than an inadvertent mistake that most insurers are willing to correct.
Amass an arsenal of reimbursement data
While the subject of bargaining with health plans may make you think of psychological gamesmanship, it's a battle mostly fought with mundane data-namely, dollar figures for billing codes. Going into negotiations well-armed will give you the confidence to face down a billion-dollar insurer, says practice management consultant David Scroggins in Cincinnati. "Conviction comes from knowledge."
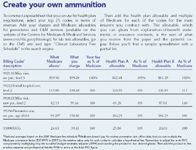
First, use your practice management program to generate a list of your top 25 billing codes in terms of dollar volume. In the 13-doctor Primary Care Associates of Northeast Ohio in Kent, OH, for instance, CPT 99213 for a level 3 office visit for an established patient topped the list in 2006, with roughly $70,000 in revenue per doctor, says internist Scott Rigby.
The second column of the spreadsheet should list the Medicare allowable for each code. These figures are essential because private payers typically express their rates as a percentage of the Medicare fee schedule-below 100 percent in hard-bitten markets and more than 150 percent in locales where physicians make a better living.
Next, create a column listing your charges for these 25 codes, followed by a column expressing them as a percentage of Medicare. Repeat that process with allowables from your top five private payers, as well as any other payer you've targeted for negotiations.
These rows and columns of numbers may show that, for some codes, the blame for poor reimbursement falls on you. If an insurer is paying your fee in full, that's a sign that you're undercharging. This happens when your fee is under or slightly above the Medicare allowable, and the insurer is willing to pay a higher multiple. Before you launch into negotiations, bring your fee schedule up to market levels. At the very least, you should set a Medicare multiple that tops the fee schedule of your best payer.





