Article
Practice Beat
Reimbursement, Stark Laws, Payment Disputes, Health Benefits, Cookbook Medicine, Medicare, Malpractice Litigation
Practice Beat
By Joan R. Rose, Senior Editor
Reimbursement: The Feds agree with you: Medicare's formula misses its goal
Don't be surprised to see another change in the way HCFA calculates your Medicare fees. In its latest report to Congress, the Medicare Payment Advisory Commission recommends replacing the sustainable growth rate (SGR) system, which is based on expenditure targets, with one "that better accounts for the cost of providing care." Medicare has been using SGR since the passage of the Balanced Budget Act of 1997. Now the commission has found that it doesn't fully account for changes in the cost of providing physician services.
Part of the problem with expenditure targets, the report notes, is that overall spending is influenced by many factors that are difficult to measurepatient and provider preferences, the diffusion of technology, and the aging of the population, for example.
But even if those problems could be overcome, it's unlikely that a mechanism like SGR could work as Congress intended, the commission concludes. That's because SGR doesn't reward individual physicians who reduce the volume of services they provide; payment increases are distributed among all physicians who care for Medicare beneficiaries.
Stark Laws: This hospital chain's generous reimbursement caught the Feds' eye
The US Department of Justice has joined a lawsuit that accuses Santa Barbara, CA-based Tenet Healthcare of violating the False Claims Act and the Stark self-referral statutes. According to the complaint, since 1993 Tenet has paid certain physicians employed by one of its Florida hospitals more than the fair market value for services in order to induce referrals.
The Stark law prohibits physicians from referring Medicare patients for certain servicesincluding clinical laboratory, and inpatient and outpatient hospital servicesto an entity with which the doctor has a financial relationship. But the statute exempts physicians employed by a hospital, as long as the doctors are paid at fair market rates and their compensation isn't affected by the volume or value of their individual referrals. Under provisions of the statute, Medicare is entitled to recover all of the revenue the hospital received from referrals made by doctors who were overpaid.
Payment Disputes: This state will hire independent arbitrators to settle doctors' beefs
In the past, when Florida physicians were unhappy with a health plan's payment decisions, they could try to settle their differences by using the HMO's arbitration process, or by going to court. Now, under a new state law, doctors can appeal adverse decisions to an independent third party for resolution within 60 days. The loser will pay the costs.
The new law also extends the protections offered under the state's existing prompt-pay law. For instance, it limits a health plan's right to retroactively deny payment for a covered service. An HMO will be allowed to deny reimbursement only if it determineswithin one year of the payment datethat the patient wasn't an eligible member.
When that is the case, the HMO may not recover its money by withholding payments for other services, unless the physician approves. If the doctor contests the repayment, the HMO can request mediation.
The law, which took effect in January, applies to noncontracting as well as contracting physicians.
Health Benefits: Skittish about the future, more employers consider bailing out
Now that consumer backlash is hampering managed care's cost-control efforts, many employers are rethinking their approach to health care, according to a survey by management consulting firm Hewitt Associates. Moreover, businesses are worried about legislative attempts to permit malpractice suits against employers who sponsor health plans. If such laws were enacted, nearly half the respondents would be apt to discontinue coverage. Last year, when the question was whether they'd definitely stop offering it, 36 percent of those polled said Yes.
Employers are evaluating new solutions and alternatives to delivering health care, says Jack Bruner, leader of Hewitt's health management division. The majority want nothing more than to "provide basic access to care at the lowest, practical cost."
In that regard, 54 percent would support changing the tax code to provide an individual tax credit for the purchase of health insurance. That's up 14 percentage points from last year.
A majority of respondents are considering the addition of consumer-driven options, such as self-directed plan designs and multitier networks. Most respondents (85 percent) believe these changes would help them get a handle on costs; 30 percent believe they would also limit employers' liability.
More than 600 US companies participated in Hewitt's survey.
Cookbook Medicine: Minnesota health plans will test a new batch of treatment recipes
Five of Minnesota's largest health plans are coming together to promote the use of evidence-based protocols for dozens of common ailments, including atrial fibrillation, congestive heart failure, diagnosis of chest pain, hypertension, degenerative disease of the knee, and lipid disorders.
Blue Cross and Blue Shield of Minnesota, Medica, PreferredOne, and UCare Minnesota have agreed to sponsor the Institute for Clinical Systems Improvement, a quality-improvement consortium that developed the standards. Until now, HealthPartners had been funding the institute by itself.
The guidelines are updated every 12 to 18 months by practicing physicians and other health care professionals. Their recommendations are based on current medical research, their own practical experience, and their knowledge of patient preferences.
The ICSI protocols can be downloaded from the Internet at www.icsi.org.
Medicare: Will Bush's proposed budget doom the Medicare program?
The Medicare Hospital Insurance Trust Fund would become insolvent in 201015 years sooner than currently projectedif President Bush's proposed budget is enacted, warns consumer advocacy group Families USA. "The President's budget plays a shell game with more than half a trillion dollars of Medicare funds," says Executive Director Ron Pollack. "At the end of that game, the [fund] is bankrupt and [its] losses helped to finance almost one-third of the President's proposed $1.6 trillion tax cut."
The report challenges the administration's contention that the budget "spends every penny of Medicare tax and premium collections over [the] next 10 years only on Medicare." In actuality, Families USA says, the President's budget would divert $526 billion over the next 10 years from the Part A Trust Fundwhich is funded by dedicated payroll taxesto cover a portion of Part B services. Those, by law, are mostly funded through general revenues, of which 25 percent comes from beneficiaries. That theoretically frees up $526 billion in general revenues to pay for other budget items, including Bush's proposed tax cut. In addition, the group notes, that diversion would result in lost interest payments of approximately $172.5 billion over the same period.
Instead of posting a surplus of $592.7 billion in 2011, the report concludes, the trust fund would be $105.8 billion in the hole.
Malpractice Litigation: Plaintiffs lose more oftenbut when they win, they win big
Although jury verdicts in medical malpractice suits increasingly favor physicians, juries appear more willing to hand down megabuck awards when the verdict goes the other way, according to Jury Verdict Research's latest study. Plaintiffs' shares of favorable verdicts declined 2 percentage points in 1999, but the proportion of million-dollar jury awards increased 6 percentage points. And while the proportion of cases involving punitive damages has remained low (3 percent in 1999), it's the highest reported in the seven-year period analyzed (1993-99).
The news on the settlement front is no brighter. The median settlement jumped 30 percent in 1999, to $650,000.
Doctors can take heart, though, that the time it takes to resolve a claim is steadily declining. The median number of months from incident date to trial was just 45 in 1999, down from 52 a year earlier. And the median number of months from lawsuit filing date to trial dropped from 28 to 25.
How malpractice payouts have climbed...
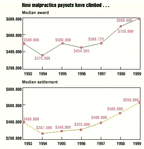
Which injuries accounted for the most 1999 verdicts...
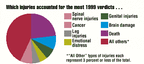
And which triggered the highest payouts in 1999
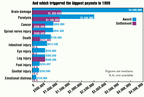
Source: 2000 Current Award Trends in Personal Injury by Jury Verdict Research
Joan Rose. Practice Beat. Medical Economics 2001;8:27.





