Article
How your productivity is measured
If you're paid based on your output, you should find out what goes into the calculation, and whether the formula is best for you.

Key Points
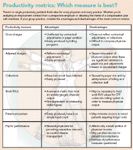
Likewise, you have your choice of stats for defining physician output.
For soloists, productivity is easy to describe-see enough patients and render enough services to meet overhead and provide you with a desirable income. In a group, however, splitting revenue is often complicated and contentious, because somebody's bound to think that the yardstick for productivity is unfair.
Some yardsticks are more equitable than others
Gross charges: This reflects the fees you charge for your services, regardless of who's paying the bill, how much an insurer might discount it, or how much is actually collected. Accordingly, this method creates no incentive to cherry-pick patients on the basis of insurance coverage, provided that a group has a consistent method for setting fees, says Denver healthcare attorney Bruce Johnson, co-author of Physician Compensation Plans and a consultant with the Medical Group Management Association. "You can't allow an individual doctor to set his fees higher than his specialty peers."
The downside to gross charges? Since fees vary from group to group and from year to year within a group, it's hard to use this metric to compare compensation packages, Johnson says. Furthermore, many doctors view gross charges as funny money-they don't reflect contractual adjustments, and they're uncollected to boot. "You can't buy a loaf of bread with gross charges," he says.
Adjusted charges: This measurement attempts to turn gross charges into a more meaningful number by subtracting third-party adjustments. However, it adds the potential for unfairness, because discounts vary by payer, and payer mix can vary markedly from one physician to another.
Consider a suburban practice that operates a satellite office in an area with a heavy concentration of Medicaid patients. A doctor in the satellite office would fare poorly under a payment system based on adjusted charges because Medicaid discounts its fees more deeply than the private insurers that dominate the payer mix at the main office.
When doctors in the same group draw upon the same patient mix, adjusted charges become a more accurate productivity metric. But even in the same office, a productivity measure that's dependent on payer mix can be easily manipulated. "In some practices, new or 'unassigned' patients with good insurance mysteriously end up with senior doctors and the Medicaid patients end up with junior doctors," Johnson notes.
Then there's the case of Dr. X, who played a dirty trick on his colleagues in a group of spine surgeons. He bribed the scheduler to send him new patients with the best-paying insurance plans.
This example of cherry-picking, encountered by Chicago practice management consultant Karen Zupko, illustrates why you need to understand how practices measure and reward physician output. The surgeons, who used collections as their yardstick, "defined productivity in a way that penalized doctors who worked just as hard as Dr. X but whose patients had stingy health plans," Zupko says.
Collections: This is the most common yardstick for productivity, largely because it's the most intuitive-it only counts money in hand. But collections can misrepresent a doctor's true productivity even more than adjusted charges because the total reflects not only the payer mix, but the practice's ability to collect the money, which may be subpar.





