Article
What would you do? If a colleague admits fraud
In an earlier issue we told you of a doctor who committed Medicaid fraud. Should he lose his hospital privileges? Here's how readers voted.
What would you do?
If a colleague admits fraud
In an earlier issue we told you of a doctor who committed Medicaid fraud. Should he lose his hospital privileges? Here's how readers voted.
By Berkeley Rice
Senior Editor
Last month, Colorado FP Renate G. Justin wrote about a colleague who had been charged with Medicaid fraud.* The medical staff at his hospital met to discuss his status. At that meeting, Jim Brown (not his real name), a respected, board-certified ob/gyn, admitted that he'd billed Medicaid twice for each office visit "so that I would break even." Then he left the room while his colleagues debated his fate.
Some argued that billing fraud simply couldn't be tolerated, and that Brown should be dropped immediately from the staff. Others felt his actions were somehow justified, since he accepted all Medicaid patientsunlike many of his colleaguesand had only tried to cover his overhead. Some argued that staff privileges should be based only on medical competence, not moral behavior. Besides, they pointed out, Brown had only been charged with a crime at that pointnot yet convicted, or disciplined by the state medical board.
We ended Dr. Justin's story without telling you the medical staff's decision, and asked you to tell us what you would dorevoke Brown's privileges, do nothing and let the courts and the state medical board deal with the problem, or suspend him temporarily until the state board decides whether to take action. After heated debate, Brown's staff colleagues voted to suspend his privileges, pending state board action. He was ultimately convicted of Medicaid fraud, and the medical board then revoked his license.
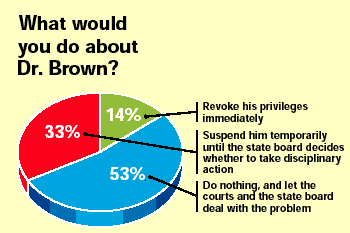
One-third of our respondents chose the same course of action. The majority53 percentvoted to do nothing, letting the courts and the state board deal with the problem. Only 14 percent chose the harshest alternative of immediate revocation of hospital privileges.
A number of physicians weren't content to simply check a course of action. They wrote or e-mailed comments. Several urged caution in such situations. As Arnold Wax, a Las Vegas oncologist, wrote: "An accusation is just that. In this country, a man is innocent until proven guilty. Only then should his privileges be revoked."
Leslie Reese, a retired gastroenterologist in Amarillo, TX, stressed the importance of "observing the due process rights of the accused, no matter how egregious his alleged transgression. Failure to do so exposes the hospital and each physician involved to the full wrath of the plaintiffs' bar." The correct response, said Reese, is to "read the hospital's medical staff bylaws carefully, and follow them to the letter, with legal advice at every step."
A Pennsylvania pathologist wrote: "If Brown's privileges were revoked or suspended, he would have a solid case against the medical staff. Besides, the medical staff generally has no authority to suspend or revoke privileges. It may recommend such action, but usually only the hospital's board of trustees has such authority. Even then, Brown should still have the opportunity of an appeal, per the bylaws. This was a case of premature expulsion."
Thomas Eans, a family practitioner in Little Rock, AR, had harsh words: "Those who participated in condemning him without a proper hearing would be liable for damaging his reputation and his businessone with which some of them are in competition. Clearly, the staff of that hospital should defer their decision until the medical board's action, if any, and then think very carefully about whether they are committing hypocrisy or inconsistency in enforcing their staff rules and bylaws."
A Texas doctor, however, took a different position: "Since Dr. Brown admitted he'd broken the law, to allow him to continue to practice might put his hospital and his colleagues in some legal jeopardy. Until his legal problems are resolved, he should remain under restriction or suspension."
One reader noted the irony of the entire situation: "Whatever Brown's fraud may have been, it is far outweighed by the fraud inherent in a Medicaid system that expects him to render care at an out-of-pocket loss."
*See "What would you do? Fraud and hospital privileges," June 6, 2003.
Berkeley Rice. What would you do? If a colleague admits fraud. Medical Economics Jul. 25, 2003;80:42.





