Article
What would you do? Alternative medicine
Author(s):
For most doctors, our poll shows, patient autonomy is key when the patient turns away from conventional medicine.
Frank, a 55-year-old teacher, has colon cancer that has metastasized to several lymph nodes and extends through the middle tissue layers of the colon wall. In addition to resection, he has undergone two rounds of chemotherapy. He says that he found the side effects of chemotherapy intolerable, and he wants to be treated instead at an alternative center that rejects what its founders call "toxic" treatments in favor of "natural" remedies, including chiropractic, whole-grain diets, and meditation. After acknowledging that his oncologist has expressed disapproval of the alternative treatments, Frank asks you, his primary care doctor, to serve as a collaborative physician with the alternative center.
If you were Frank's doctor, what would you do?
That's what we asked when we posed this and four other modern-day ethical dilemmas in our Aug. 18 issue.
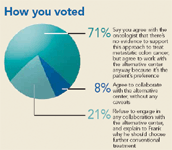
Another 8 percent of respondents would oblige Frank without any qualifications or admonitions; 21 percent would steer totally clear of any involvement with unproven treatment approaches. One respondent-respondents were given the choice of being quoted by name or remaining anonymous- who would do the former puts it bluntly: "I can't force patients to deviate from their beliefs in the name of science. Besides, in some instances, chemotherapy is little better than a placebo." J. Jeffrey Morrison, an FP in Spartansburg, SC, would steer clear entirely because "I can't make the patient submit to proper treatment, but I can avoid helping him get improper treatment."
Opting for patient choice
A number of those who say they'd work with the alternative treatment center see that option as the best way of ensuring that Frank stays at least partly within the confines of conventional medicine. An internist who expresses that sentiment writes, "Option 3 [refusing to work with the alternative center] is likely to result in Frank leaving my practice. With option 1 [expressing your misgivings, but agreeing to Frank's request], I might be able to persuade him to continue with conventional treatment, as well." And San Diego cardiologist Allen Jay notes, "Among the reasons that the primary care physician should attempt to maintain rapport with the patient is that if a new, more effective conventional treatment becomes available, the patient might accept."
Among the other reasons respondents would do as Frank asks:
To be there if the illness worsens. "As the metastasis persists, he's going to need me once he enters hospice," says Pat Conrad, an emergency physician in Niceville, FL. Chicago internist Paul Lorensen expresses a similar view: "The patient has enough problems and will need my continued support. Also, if the prognosis is as grim as the history suggests, discontinuing chemo might be a feasible option. Should that happen, an alternative center might allow the patient to feel that something was being done for him."





