Article
UPDATE: Focus on Practice
NP competition; more tort reform; HIV organ donations; EHR boost
Some HIV patients can now donate organs
Illinois recently became the first state to allow HIV-infected patients to donate organsalbeit only to similarly infected patients. In addition to providing an expanded base of available organs, the new law "will enable people with HIV to live longer, healthier, more-productive lives," says Illinois Gov. Rod R. Blagojevich. Illinois, like many other states, previously required organs infected with HIV to be destroyed.
Leading doctors into the information technology age
Responding to the Bush administration's push for widespread adoption of electronic health records, 14 medical organizations have joined to educate physicians about EHRs' value and how they can best be used. The Physicians Electronic Health Record Coalition, which represents more than 500,000 US physicians, plans to help doctors determine which system best suits their needs and assist them in finding high-quality, affordable products. The group will focus primarily on small- and medium-sized ambulatory care practices.
Meanwhile, a survey conducted this summer by the American Academy of Family Physicians (a coalition member) found that a surprisingly high 40 percent of the 788 FPs responding had completely converted to EHRs or were in the process of doing so. Nearly three-fourths of those with systems in place believe that the technology enabled them to reduce prescribing errors and improve communication.
Medical errors: More widespread than believed?
An average of 195,000 inpatients died annually from preventable medical errors that occurred from 2000 through 2002, according to a new study. That's nearly double the number noted in the oft-cited 1999 Institute of Medicine report. The latest study, conducted by HealthGrades, a quality rating company, involved 37 million Medicare patient records nationwide. Researchers analyzed the quality of care based on 16 patient-safety indicators as defined by HHS' Agency for Healthcare Research and Quality. They concluded that almost 75 percent of all mortality attributable to patient safety incidents was the result of failures to diagnose and treat in time and to unexpected death in a low-risk hospitalization.
The tort reform tug-of-war enters a new arena
Come November, voters in several states will consider constitutional amendments related to medical malpractice. In Florida, where doctors and lawyers are in a heated battle, an initiative backed by the state medical society would limit the contingency fees lawyers receive. Trial lawyers, meanwhile, have floated two propositions. One would allow current and prospective patients to obtain information about adverse incidents involving a physician; the other would deny licensure to any physician found to have committed malpractice three or more times. If passed, the law would be retroactive and exclude settlements.
Meanwhile, two statesOregon and Wyominghave constitutional amendments that would cap damages. Wyoming residents will also decide whether to require alternative dispute resolution or a medical panel review before a person files a malpractice lawsuit. In addition, in Washington, the state medical society has filed an initiative to force lawmakers to address tort reform. Noneconomic damages and attorneys' fees would be capped, awards would be paid out over time, and juries would be told of other compensation the injured patient has received or will receive from another party. If the legislature fails to act during the session that begins in January, the measure will go before voters in the fall of 2005.
New competition from NPs?
Pending New York State approval, Columbia University's School of Nursing plans to offer a doctoral degree for advanced practice nurses. The Doctor of Nursing Practice (DrNP) program will prepare candidates for independent care. The program would include classroom courses, supervised practice, and residency. Graduates would then be able to care for patients in an outpatient office, evaluate their needs in the ED, admit and co-manage hospitalized patients, provide advice and treatment over the phone while taking call, initiate specialist referrals, and evaluate the subsequent advice. The post-master's program would be two years, including one year of residency, while the post-baccalaureate program will be four years, plus one year of residency. The DrNP could be conferred in any specialty of advanced practice.
While the AMA supports collaborative practice between NPs and physicians, the organization opposes independent practice. Moreover, the combination of Dr and NP is likely to be confusing to patients, says AMA Trustee Rebecca Patchin.
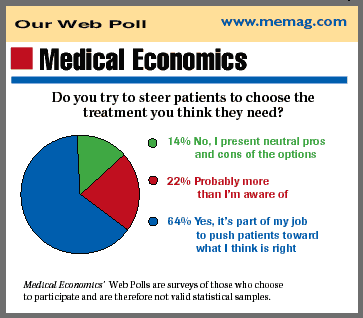
Our Web Poll
Joan Rose. UPDATE: Focus on Practice. Medical Economics Sep. 17, 2004;81:12.





