Article
UPDATE: Focus on Practice
FPs in demand; higher Medicaid fees
Reading new meaning into the duty to care
Breaking with tradition, the Arizona Supreme Court ruled that a physician may have a duty to care even if a formal doctor-patient relationship doesn't exist. The case involved a radiologist who found abnormalities (a small nodule and a patchy consolidated parenchymal pattern) in an X-ray taken as part of a nurse's pre-employment physical for tuberculosis. Although the doctor's observations were forwarded to the nursing home that had hired him to screen the would-be employee, he didn't disclose his findings to the nurse. The physician not only "should have anticipated" that the woman would want to know of the potentially life-threatening condition, the court said, but also should have recognized that "not knowing about it could cause her to forgo timely treatment."
The case now goes back to trial court.
FPs are in vogue again
Since 1997, demand for specialists has been steadily increasing while the need for primary care physicians has declined, especially in the field of family medicine. However, in a striking turn of events, FPs now rank among the top five most-wanted physicians, reports Merritt, Hawkins & Associates, a Texas-based physician recruiting firm. During the 12 months ending March 31, MHA saw a "significant spike" in searches for FPs from the previous 12 months. MHA notes, however, that the average income offered doesn't yet reflect the seemingly renewed interest in family physicians.
What potential employers
are willing to pay FPs
California's play-or-pay law is up for grabs
A referendum on the November ballot in California seeks to block implementation of a law that would require employers in the state with 50 workers or more to provide health insurance for their employees. The law, which isn't scheduled to go into effect for a couple of years, requires employers who don't provide a minimum set of health benefits to purchase coverage through the state. The law also calls for all group health insurance policies sold in California to include prescription drug coverage.
Higher Medicaid fees, but not for long
Contrary to most of the 1990s, when physicians' Medicaid fees grew very little, fee-for-service reimbursement rose 27 percent on average from 1998 through 2003, according to a recent study. Primary care physicians posted the largest gains41 percent. However, because Medicaid reimbursement continues to lag behind that of other insured groups, doctors in states where reimbursement is lowest are less willing to accept new Medicaid patients, researchers say. Now, caught in a new budget crunch, states are once again freezing or reducing fees. That puts access to care at even further risk, researchers warn.
The study appears on the Health AffairsWeb site.
For these doctors, quality care pays off
Blue Cross of California paid $56.9 million in bonuses to 134 physician groups that participate in its HMO Quality Scorecard initiative. This is the second year that Blue Cross has rewarded physicians for improving the quality of care provided to non-Medicare HMO patients. Last year, 80 physician groups earned $28 million in bonuses.
Medical groups are judged on three main areas of performance: clinical quality (which accounts for 50 percent of the score), patient satisfaction (40 percent), and investment in information technology (10 percent). The quality measures include patient satisfaction survey results, waiting times for appointments, number of complaints and grievances, peer and staff reviews, and patient turnover. Groups were also tracked on how well they manage chronic diseases (such as asthma and hypertension) and adhere to screening guidelines for breast and cervical cancer.
The FTC's crackdown on physicians continues
Without admitting wrongdoing, Southeastern New Mexico Physicians IPA, a 68-doctor group in Roswell, and two nonphysician employees have agreed to settle FTC charges that they increased patients' healthcare costs by fixing prices. The agency charged that the physicians refused to deal with health plans on an individual basis. Instead, the two employees negotiated fees and other terms, and refused (or threatened to refuse) to deal with those plans that wouldn't meet the doctors' terms. The group includes 73 percent of the area's doctors in private practice.
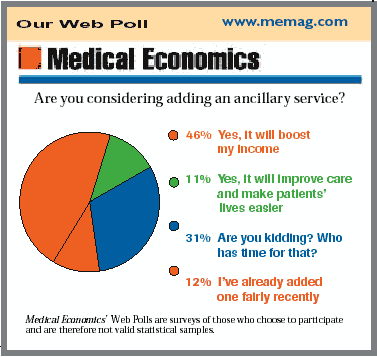
Our Web Poll
Joan Rose. UPDATE: Focus on Practice.
Medical Economics
Aug. 20, 2004;81:9.





