Article
UPDATE: Focus on practice
Questionable codes; Cigna settlement
UPDATE
Focus on Practice
By Joan R. Rose
Uncle Sam's latest move to reduce overbilling
CMS has posted the automated edits used to identify questionable Medicare claims and to adjust payments on its Web site (cms.hhs.gov/physicians/cciedits). The edits, known as the National Correct Coding Initiative, identify pairs of services that normally shouldn't be billed by the same physician for a single patient on the same day. Previously, the edits were available to physicians only on a subscription basis. Earlier this summer, CMS added the Medicare Physician Fee Schedule Look-up to its Web site, (cms.hhs.gov/physicians/default.asp), making it possible for physicians to determine in advance what they will be paid for a particular service or range of services.
Seniors cool to Medicare drug benefits
Three out of five respondents to a Kaiser Family Foundation/Harvard School of Public Health poll want Congress to add a prescription drug benefit to Medicare this year. Surprisingly, seniors (age 65 and older) are less supportive of the idea than younger respondents (54 vs 62 percent). More than three-fourths of senior respondents are worried that they will still pay too large a share of their drug billsa worry that eclipses all other concerns by a wide margin.
Is your patient's insurance valid?
Rising health care costs and increasing numbers of uninsured have spawned an unprecedented increase in unauthorized and illegal health insurance plans, according to a new report from The Commonwealth Fund. Since 2001, four unauthorized plans have left nearly 100,000 people with no health coverage and approximately $85 million in unpaid medical debts. While no state is immune to the problem, Florida and Texas have been especially hard hit. In the last two years, insurance scams have claimed 50,000 victims in those two states alone.
Operators of these scams often sell coverage through professional and trade associations, phony unions, and professional employee organizations. "Being victimized by a phony health insurance scam is worse than being uninsured because the victims are not only stuck with huge medical bills, they've also been defrauded of thousands of dollars in premiums," says Mila Kofman, a co-author of the report.
Cigna settles at long last
Cigna HealthCare has reached a settlement with some 700,000 physicians involved in the mammoth class-action lawsuit pending in US District Court in Miami. The agreement, which requires the company to institute new business practices, has received preliminary approval from the court.
In addition to monetary relief (estimated at more than $700 million), Cigna has agreed to adjust fee schedules only once a year and to keep payment rules consistent across all types of health plans. The health insurer will make capitation payments from the time a patient chooses a primary care physician or is assigned to one. Moreover, it will drop its requirement that doctors who participate in one of its health plans must participate in all of them. The agreement also addresses a variety of other issues, including the definition of medical necessity, an external review system for physician disputes, CPT reimbursement coding edits, and the end of automatic downcoding.
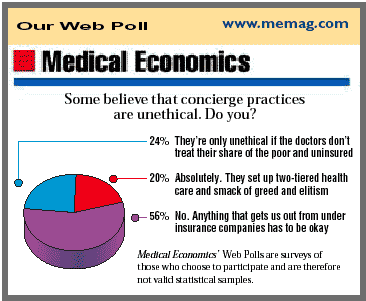
Our Web poll
Joan Rose. UPDATE: Focus on practice. Medical Economics Oct. 24, 2003;80:10.





