Article
UPDATE
Author(s):
On finance and practice
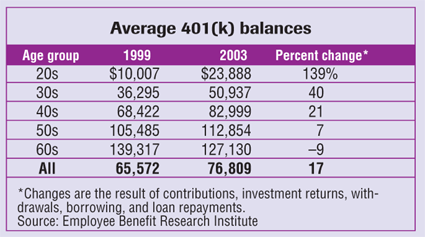
FOCUS ON FINANCEDo my own taxes?! I'd rather clean the garage Most physicians-around 87 percent-hire an accountant or tax attorney to do their taxes, according to a recent Medical Economics poll. A little less than 8 percent of MDs and DOs say they tackle this chore themselves, while around 4 percent allow their spouse the pleasure. Among all physicians surveyed, doctors between the ages of 30 and 34 were the least likely to use an accountant or tax attorney (just 72 percent of respondents use one or the other), while those 60 to 64-who presumably have more-complicated finances than their younger colleagues-are the most likely to call on a tax pro (94 percent).
Internists were the most likely to do their own taxes, with a plucky 17 percent reporting that either they or a spouse handle them. On the other hand, just 3 percent of orthopedic surgeons said they do the job themselves.
The poll of 8,159 physicians is part of Medical Economics' exclusive annual survey of physicians' compensation, expenses, and attitudes.
Are mpg ratings accurate? The EPA is considering a change in how it calculates fuel efficiency ratings for new passenger vehicles. Bluewater Network, a nonprofit environmental group, petitioned for action, arguing that the EPA's miles-per-gallon ratings overstate actual performance by as much as 34 percent. The group says the EPA's tests, last updated in 1984, are based on an average highway speed of 48 mph, underestimate the amount of stop-and-go traffic, and assume that drivers aren't running the air conditioner.
The SEC goes to bat for individual investors A new SEC ruling bans directed brokerage commissions, in which mutual fund companies reward brokers who sell their funds to clients. The payments, which are often hidden from investors, represent about 20 percent of annual fund expenses. Consumer groups, including Fund Democracy and Consumers Union, say the rewards create a conflict of interest for brokers, who should sell mutual funds because they're appropriate for their clients, not because of the commission they carry.
A second recent SEC ruling requires fund companies to reveal more information about who exactly is in charge of their portfolios, and whether the managers invest their own money in the fund. Fund companies must disclose the names of the top five fund managers and a brief description of their role on the management team, in place of the current practice of simply listing funds as being "team-managed." To help investors determine whether fund managers share their financial interests, mutual funds also have to indicate, within ranges, how much managers have invested in the portfolios they oversee and what kinds of bonuses they earn.
Check your wait time for airport security A new Web site can give you an estimate of waiting times at security checkpoints at any commercial airport in the country. The Transportation Security Administration gives estimates for average and maximum waiting times for the day and time you select (waittime.tsa.dhs.gov). The estimates are based on averages for the previous 28 days, and relate strictly to security delays. They won't reflect delays caused by bad weather, holiday crowds, packed parking lots, or long ticketing lines.
FOCUS ON PRACTICEA major purchaser plays health plan hardball The California Public Employees' Retirement System has won state approval of a plan to cut its ties with 25 hospitals. CalPERS decided in May not to renew contracts with 38 of the most expensive hospitals in the Blue Shield HMO network next year. The move had been estimated to save the pension fund about $36 million in 2005 and $50 million annually thereafter. Since then, 10 hospitals have agreed to bring their prices in line with the statewide average and have rejoined the provider network. The state Department of Managed Health Care, which reviewed the plan to ensure that CalPERS' 1.2 million members would have adequate access, restored four others.
Hospitals take a pass on buying practices Few hospitals today are interested in owning and managing medical practices. According to the 2004 Goodwill Registry, hospitals purchased just 4 percent of practices sold last year-down from 19 percent five years ago. Solo physicians bought the majority of available practices (83 percent), while group practices took ownership of another 11 percent.
The registry, managed by The Health Care Group of Plymouth Meeting, PA, is a national database of goodwill values compiled from actual transactions.
Managed care: It's déjà vu all over again With premiums still rising at double-digit rates, some health insurers have begun reintroducing cost-control measures that triggered a managed care backlash during the 1990s, according to an article published on Health Affairs' Web site. Among the unpopular strategies making a comeback: preauthorization for outpatient services and specialist referrals, physician utilization review, higher out-of-pocket expenses, steering patients to more cost-effective providers, and concurrent and retrospective review of inpatient services. Moreover, several plans introduced concurrent review to their PPOs in 2002-2003, although that practice previously had been limited to HMOs. Insurers are also experimenting with new plans that offer a more limited choice of hospitals and physicians than is available in standard HMOs and PPOs.
Access the report online at http://content.healthaffairs.org/cgi/content/abstract/hlthaff.w4.427
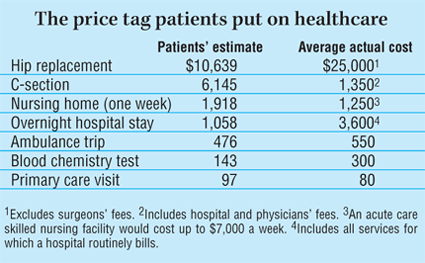
Are patients immune to the cost of care? The move toward consumer-directed healthcare assumes that patients will be knowledgeable enough to make prudent decisions on how to spend their healthcare dollars. However, a new Wall Street Journal Online/Harris Interactive poll of 2,366 adults suggests that patients aren't cognizant of the true cost of care. For example, respondents overestimated by 21 percent the cost of a primary care office visit and underestimated by 71 percent the cost of an overnight hospital stay.
Residents' class-action suit gets tossed Citing a new federal law exempting the National Resident Matching Program from antitrust laws, a federal judge has thrown out a restraint-of-trade lawsuit filed against the NRMP, the Association of American Medical Colleges, the Accreditation Council for Graduate Medical Education, and 27 teaching hospitals. The suit, filed in May 2002 and brought on behalf of 200,000 resident physicians, charged that the matching program violates antitrust laws by preventing competition for residents' services, artificially depressing and standardizing wages below competitive levels, and conspiring to establish rules that accredit and govern residency programs.
The NRMP, which was created in 1952, uses a computer algorithm to match graduating medical students to residency programs. According to the AAMC, the "Match" prevents a "frenetic free-for-all, involving thousands of students and thousands of residency programs scrambling simultaneously to find their best options."
Getting appropriate care sometimes means long waits Access to specialty care is becoming more problematic for Americans, according to a recent survey. On average, new patients wait more than 30 days to schedule an office visit in some metropolitan markets, and some wait as long as 50 days. The survey focused on four medical specialties: cardiology, dermatology, obstetrics-gynecology, and orthopedic surgery. All four specialties reported three days as the shortest wait. The longest wait was 81 days, which dermatology patients had to endure.
Texas-based Merritt, Hawkins & Associates, a national physician search and consulting firm, conducted the telephone poll that examined 1,062 physician offices in 15 major metropolitan areas.