Article
Practice Beat
Author(s):
Provider Panels; Prompt Payment Laws; Reimbursement; Professional Liability
Practice Beat
By Joan R. Rose, Senior Editor
Provider Panels
Court to managed care plans: no more no-cause boots
Managed care plans cannot arbitrarily dismiss physicians from their provider networks, even when the agreed-upon contract permits no-cause terminations, the California Supreme Court has ruled. "If participation in managed care arrangements is a practical necessity for physicians generally, and if only a handful of health care entities have a virtual monopoly on managed care, removing individual physicians from preferred provider networks controlled by these entities could significantly impair those physicians' practice of medicine," the court reasoned.
The case in question arose in 1992, after ob/gyn Louis E. Potvin was booted from MetLife's provider network. Under the terms of his contract, either party could terminate the relationship without cause with 30 days' written notice. The physician argued that he should have been given reasonable notice and an opportunity to be heard before his removal.
Two years after he signed on, MetLife notified Potvin that he was being terminated. When he pressed the insurer for an explanation, MetLife cited his malpractice history. The doctor had practiced medicine for more than 35 years, was a past president of the Orange County Medical Association, and held full staff privileges at Mission Regional Hospital (where he had served as chairman of the obstetrics and gynecology department for nine years). But he'd been sued for malpractice four times. Three of the cases were dropped, but the fourth was settled for $713,000. All predated his 1990 contract with MetLife. Under the insurer's selection and retention standard, however, physicians with more than two suits or aggregate payouts exceeding $50,000 were excluded from its network. When Potvin's request for a hearing went unanswered, he sued.
The doctor argued that the public policy considerations supporting the common law right to fair procedure render the "without cause" clause in the MetLife preferred provider agreement unenforceable. And he claimed that his removal from the insurer's panel had devastated his practice and resulted in his rejection by "physician groups that were dependent upon credentialing by MetLife."
MetLife countered that, even if removal of a physician from its preferred provider lists is subject to the common law right to fair procedure, Potvin had waived that right by agreeing that the insurer could terminate the arrangement without cause.
While agreeing with Potvin that the "without cause" clause violated the contractual obligations of good faith and fair dealing, the high court nevertheless pointed out that its holding doesn't prevent an insurer from dropping a physician without regard to its effect on his finances, as long as the decision is "substantively rational and procedurally fair."
"The common law right to fair procedure does not apply . . . unless the insurer possesses power so substantial that the removal significantly impairs the ability of an ordinary, competent physician to practice medicine or a medical specialty in a particular geographic area, thereby affecting an important, substantial economic interest," the court explained.
Prompt Payment Laws
Giving doctors recourse when HMOs don't pay
Physicians in New Jersey may soon find it easier to resolve complaints over slow or late payments. Under proposed regulations to implement New Jersey's Health Care Information Networks and Technologies Act (HINT), insurance carriers and HMOs would have to establish a two-tiered appeals process similar to that used to settle disputes over medical decisions. The system would provide an independent external appeals process for settling disagreements that an internal review couldn't resolve. "Late payment costs everyonedoctors, hospitals, insurers, and consumers," says Gov. Christine Whitman. "Physicians fight diseases. They shouldn't have to fight insurance companies and HMOs."
When implemented, HINT will require that claims filed electronically be paid in 30 days (instead of the current 60), and paper claims would have to be paid within 40 days. Insurers who decide to contest a claim would have only 30 days instead of 90 in which to do so. The law also establishes time frames for carriers to acknowledge the receipt of a claim. To get a handle on claims payment patterns, New Jersey's acting banking and insurance commissioner has ordered all state-regulated insurance carriers and HMOs to review their payment practices going back to January 1998 and report that data to the state.
Reimbursement
Physicians may find these plans more to their liking
The Health Care Financing Administration has approved a request by Sterling Life Insurance to offer a private fee-for-service health plan option for Medicare beneficiaries. Under the plan, to be available primarily in rural areas, enrollees will be covered for all Part A and Part B services as well as worldwide emergency care and more inpatient days. In addition to a premium, beneficiaries will have higher out-of-pocket expenses, but generally will pay less to see a doctor than under original fee-for-service Medicare. Physicians who choose to treat these patients will be paid on a fee-for-service basis and won't be subject to utilization review.
The new Medicare+Choice plan debuts this month in 11 statesAlaska, Idaho, Kentucky, Minnesota, Nebraska, New Mexico, Nevada, Oregon, South Dakota, Tennessee, and Utahas well as in selected counties in Arkansas, Louisiana, Mississippi, Ohio, Texas, and West Virginia. For more on the Sterling plan, check out the Washington Beat column in our next issue, July 24.
Meanwhile, in the private sector, doctors will get to set their own capitation under a plan created by Minneapolis-based Vivius. Employers will set up an annual health care spending account for each employee. The workers will then create their own provider panels (personal physician, specialists, hospital, lab, radiology clinic, and pharmacy network) and choose the level of out-of-pocket copayment they're willing to make. Vivius' Web site (www.vivius.com) will calculate the annual cost of the services selected, and patients can try several choices before finalizing their selections. Employees will also purchase a wraparound health insurance policy to cover services that their physician panels can't provide (or for out-of-network emergencies). Then, each month, Vivius will electronically transfer money from each employee's spending account to the accounts of providers selected for their panels.
"Consumers and physicians are ready for an end to 'Mother, may I?' medicine," says oncologist Lee N. Newcomer, Vivius' executive vice president and chief medical officer. This concept "gives complete decision-making rights to the patient and physician, while keeping health care costs under control." Newcomer previously was the chief medical officer and executive vice president for health policy and strategy at UnitedHealth Group.
The company will test market the plan in Minneapolis and Kansas City, MO, this fall.
Professional Liability
1998: A year when malpractice awards mushroomed
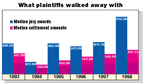
Although doctors are still likely to prevail in medical malpractice actions, awards in cases that go against them are getting bigger, according to the latest report from Jury Verdict Research. The median award for medical malpractice skyrocketed more than 46 percent in 1998to $755,530, from $515,738 in '97.
"It's difficult to tell how juries are treating medical malpractice cases," says Dave Boxold, author of JVR's Current Award Trends in Personal Injury. Plaintiffs won almost 60 percent more money in 1997 and '98, he notes, while their share of favorable verdicts declined. And doctors who settled their cases found that they had to agree to higher payouts, as well. The median settlement in 1998 was $497,412, a 24 percent jump from the previous year.
But there are some bright spots in the developing malpractice picture: Although compensatory damages are increasing, 1998 marked the first time in the '90s that no punitive damages were awarded. And the time it takes to resolve a claim (from date of incident to jury verdict) dropped from 60 to 52 months. From the date of filing to resolution, it's now 29 months, down from 37.
Outcomes most likely to result in a plaintiff verdict in 1998...
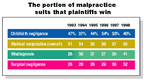
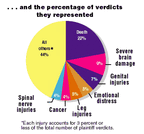
Source: Current Award Trends in Personal Injury1999 Edition
Joan Rose. Practice Beat. Medical Economics 2000;13:24.





