Article
Practice Beat
Author(s):
Hospitals, Physician Retirement, Medical Practice, Medical Marijuana, Electronic Prescribing, Report Cards, Did You Know...
Practice Beat
By Suzanne Duke, Senior Associate Editor
Hospitals
How CEOs have learned to manage managed care
Maybe there's a lesson doctors can glean from hospitals' dealings with HMOs: Just say No.
Almost a third of hospitals nationwide have canceled an HMO contract. Among those with 500 or more beds, that figure is close to 60 percent, according to Deloitte & Touche's survey of about 1,000 executives at acute care hospitals. The most common reasons for discontinuing an affiliation with an HMO: poor return on the contracts and the plans' lack of responsiveness.
What might account for hospitals' assertiveness in negotiating with HMOs? The institutions aren't as reliant on managed care as they thought they'd be. Two years ago, most CEOs surmised that HMOs would account for more than 20 percent of their business in 2000. The reality is that only a quarter of the hospitals responding to the survey say that managed care accounts for that much, and many respondents predict that the growth of business attributable to HMOs and PPOs will slow.
Physician Retirement
Why older doctors are bailing out early
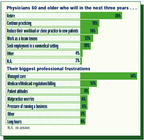
One sampling of physicians 50 years and older indicates they're voting with their feet. Tired of managed care and Mediplan hassles, more than a third are opting to retire soon, according to Merritt, Hawkins & Associates, a physician recruiting firm in Irving, TX.
Though 60 percent of the 300 physicians surveyed say they relish their relationships with patients, they have a less than sanguine outlook on medical practice. More than half found medicine to be less satisfying in the last five years, and nearly that many said they would reconsider going into the profession if they were starting out today. Even fewer doctors would encourage their children to pursue a medical career.
Medical Practice
Losing patients? Don't blame health plans
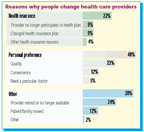
Insurers may not be driving consumers to change their doctors, hospitals, and other providers to the extent that anecdotal evidence suggests, says Marie C. Reed, an analyst for the Center for Studying Health System Change (HSC). According to a new HSC study, patients who switch doctors or hospitals are more likely to be motivated by personal preference than by health plan rules.
Twenty-two percent of patients who changed providers in 1998 and '99 did so for health insurance reasonsa statistically significant drop from 26 percent in 1996 and '97. Among patients who switched providers in '98 and '99, two in five cited personal preferences as the reasonnearly twice the number that blamed their health planswhile another 38 percent gave miscellaneous reasons for their decision.
Medical Marijuana
Hawaii's legislature and governor okay it
While ballot initiatives have legalized medical marijuana in several states (Alaska, Arizona, California, Maine, Oregon, and Washington), Hawaii has become the first state to pass a marijuana bill through its legislature.
Gov. Benjamin Cayetano has signed legislation that allows patients to use marijuana to relieve severe symptoms of cancer, glaucoma, HIV, AIDS, multiple sclerosis, epilepsy, and Crohn's disease. The law also allows those with chronic diseases who suffer from cachexia, pain, nausea, seizures, and muscle spasms to use the drug.
Under the tightly worded measure, patients must register annually with the Department of Public Safety. They may not use marijuana in public places or in moving vehicles. "If the law is abused, I will not be surprised to see a move to repeal it," the governor cautioned. "So I hope the practitioners who believe in the medicinal value of marijuana are aware of this and take precautions."
The bill's passage, however, may be a Pyrrhic victory for marijuana proponents. A recent study in the Journal of Immunology reports that THC, the major psychoactive component of marijuana, can promote tumor growth by reducing the body's anti-tumor immunity. Previous studies have found that THC can also lower resistance to bacterial and viral infections.
Electronic Prescribing
A financial incentive to embrace technology?
iScribe, a San Mateo, CA, health care technology firm, has partnered with The Doctors' Company, the country's largest physician-owned malpractice insurer, to offer discounts to physician members who use electronic prescribing software.
TDC members will receive an annual 5 percent discount on malpractice insurance premiums, up to $1,000, after they've used the iScribe system for one year. iScribe will give free prescribing softwarealong with a handheld computer, wireless printer, and customer service supportto member physicians nationwide. The Doctors' Company hopes that the software, which checks for drug interactions, duplications, and allergies, will reduce the number of medication errors. These mistakes cost nearly $29 billion a year in the United States.
In addition to its safety benefits, the software will alert physicians to formulary information, drug copayments, and costs. Prescriptions can be printed, faxed, or sent electronically with encryption to pharmacies.
Report Cards
Patients nationwide will rate your nonclinical skills
In what may be the largest study ever undertaken outside the US Census, Nebraska-based National Research Corp. will survey patients nationwide to find out how they rate the quality of their primary care physicians' nonclinical performance. Rather than focus on technical issues, the survey will elicit information on topics of more interest to consumers, such as whether the doctor answers questions patiently and explains what he's thinking.
Earlier this summer, more than 250,000 households in Cincinnati and Portland, OR, received surveys seeking information on roughly 1,750 primary care doctors. NRC will begin adding more markets early next year. Ultimately, the company hopes to rate the nation's 143,000 primary care physiciansa task that will require 15 million households to be surveyed.
The report cards will be a valuable tool for patients and physicians, says NRC President/CEO Mike Hays. Patients will have access to information that will help them find practitioners they can build relationships with, and doctors will be able to identify aspects of their service that patients find wanting.
Health plans are expected to purchase the information and provide it to potential enrollees during open enrollment periods. NRC is also negotiating with several Internet and E-health companies to post the data through links from their sites to NRC's.
DID YOU KNOW . . .
- Nearly a third of adults ages 19 to 29 have no health insurance. They're twice as likely as children and older adults to be uninsured.
- Seventy-five percent of uninsured workers in that age group don't have access to employer-sponsored health plans.
- One-quarter of young adults have below-poverty-level incomes (about $8,500 for singles and $13,000 for families of three). Health coverage for individuals in the 20 to 29 age bracket can cost more than $2,000 a year, and $5,000 for families.
- Young adults without health coverage are twice as likely as their insured counterparts not to seek medical care when they're sick. Half of the low-income young adults who go without needed care do so because they can't afford it.
Source: The Commonwealth Fund
Suzanne Duke. Practice Beat. Medical Economics 2000;16:17.





