Article
Practice Beat
Managed Care, Physician Networks, Medicare, Quality Care
Practice Beat
By Joan R. Rose, Senior Editor
Managed Care: Aetna removes one thorn in doctor's sides
Physicians who sign or renew contracts with Aetna US Healthcare this year are in for a surprise. The insurer is dropping its hated all-products clause, nationwide.
Physicians entering the network for the first time will be able to select participation in any or all of the health plans Aetna offers. Currently, participating physicians who want to opt out of the all-products requirement generally have to give the insurer written notice 90 days before their contracts come up for renewal.
Why is Aetna changing its longtime contracting requirement? Because, its officials say, they believe the policy change will spawn a more collaborative relationship with participating physicians and encourage those who don't participate to sign up.
Previously, Aetna had relaxed its all-products policy in Connecticut, Georgia, Texas, and Virginia. More recently the company agreed to do the same in California, Florida, and New Jersey.
Physician Networks: An HMO reacts to organized medicine's protest: Sorry, we goofed
A Michigan HMO's plan to cut costs by limiting patients' choice of primary care providers drew such vehement protests from physicians that the health plan has backed away from the decision.
Last fall, Care Choices HMO notified members in the Muskegon area that they could no longer designate internists as their primary care providers. Instead, members would have to choose from among the network's FPs and GPs. Internists would continue as part of the physician network, but they'd be considered specialists and patients would need a referral to see them.
In protesting the move, the American College of Physicians-American Society of Internal Medicine (ACP-ASIM) said it knows of no other insurer that fails to recognize internists as primary care physicians.
Fearing that the policy could be expanded to cover all 188,000 Care Choices members in Michiganor even to its parent organization's other health plansthe medical society argued that the new policy would disrupt continuity of care and ultimately increase health costs.
Noting that internists typically treat older patient populations with a greater prevalence of chronic disease, the ACP-ASIM questioned the HMO's motives. In particular, the group said, it would be "very concerned if the intent of Care Choices' new policy was to reduce costs and encourage these patients to disenroll from the network by denying patients with chronic diseases" the coverage to see the very physicians who are trained to treat them.
In admitting its mistake, the HMO acknowledged that the policy change had been prompted by a desire to save money. The cost of care is higher in Muskegon than in other areas, the HMO said, because of the high incidence of chronic disease in the community. The HMO has restored internists to its primary care ranks.
Care Choices is a subsidiary of Trinity Health, which has more than 40 hospitals and dozens of other health care companies in seven states. It's the third largest Catholic health system in the US.
Medicare: Think the tab is huge now? Just wait
The Balanced Budget Act of 1997 helped stabilize Medicare for the near term, but major changes will be needed to maintain its fiscal integrity and protect beneficiaries from overwhelming out-of-pocket burdens. That's the conclusion in a new study from the Urban Institute.
In particular, researchers say, the government will have to address rising overall health care costs, insufficient Medicare revenues (from payroll taxes), and the growing elderly population.
As the Medicare population increasesit's projected to grow from 40 million in 2000 to 70 million in 2025beneficiaries will experience an increasing drain on their resources for health care needs, the study warns. For example, the average annual out-of-pocket cost today for services not covered by Medicareincluding premiums, medical services, and prescription drugsis $3,142. By 2025, those expenses are projected to rise to $5,248 (in 2000 dollars), amounting to 30 percent of the average beneficiary's income.
Some segments of the population will be even harder hit, forcing them to choose between basic necessities, like food or housing, and treatment. Older low-income women in poor health, for instance, had an average out-of-pocket cost of $5,969 last year. By 2025, that will jump to $9,378, or 72 percent of their incomes.
Quality Care: What doctors think of their ability to deliver top-notch care
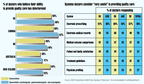
More than half the physicians in the US believe that their ability to provide quality health care has deteriorated over the last five yearsand large percentages of their colleagues in four other English-speaking nations agree, according to a recent study. Moreover, although doctors don't view the situation as irreversible, many fear that the decline in quality will continue, says study author Robert J. Blendon, professor of health policy and political analysis at Harvard University.
At least half the doctors surveyed are convinced that technologyin particular, electronic prescribing and electronic medical recordswill improve the quality of care. But they're less apt to believe that medical outcome comparisons, treatment protocols, and physician profiling are effective.
Percent of doctors who believe their ability to provide quality care has deteriorated
Systems doctors consider "very useful" in providing quality care
Joan Rose. Practice Beat. Medical Economics 2001;4:19.





