Article
Practice Beat
Timely payments, Coverage appeals, Direct-to-consumer ads, Docket watch
Practice Beat
By Joan R. Rose, Senior Editor
Timely Payments: A big setback for Michigan doctors
While more and more states are enacting prompt-payment laws, Michigan Gov. John Engler has vetoed a similar bill. The governor's action is a blow to the Michigan State Medical Society, which had lobbied hard for the measure. The bill would have required insurers to pay clean claims within 45 days or be subject to a 12 percent annual interest charge.
In vetoing the bill, Engler took issue with a provision that would have made the state's Office of Financial and Insurance Services the arbiter of contractual disputes between providers and health plans. The governor said he supports the timely payment of health care claims, but doesn't want the state government involved in contract disputes between private entities. Providers already have signed contracts that indicate how and when payments are to be made, he pointed out. He viewed the bill as a legislative attempt to micromanage existing contracts between private parties.
Moreover, Engler noted, it's inappropriate for the state government to be a bill collector for the health care industry. That's a job for the judiciary, he maintained.
To date, 40 states have enacted laws ensuring the right of providers to be paid within a specified period.
Coverage Appeals: New Jersey strengthens its patient-protection law . . .
Before leaving office to become EPA chief, New Jersey Gov. Christine Todd Whitman signed into law a measure that gives patients the right to appeal HMO disputes directly to an independent utilization review panel. Using guidelines developed by the federal government, medical organizations, and others, the panel will review the patient's medical record and render a decision within 90 days of receiving the appeal. The key element of the law: Panel decisions will be binding on insurers.
A 1997 law gave patients in New Jersey the right to take their HMO beefs to an external review panelbut only after going through a health plan's internal review process. And even if the panel found in the patient's favor, the insurer wasn't bound to pay for the disputed treatment.
. . . while California finds fault with arbitration
About 80 million Californians receive their health care through managed care plans. When treatment disputes arise, three out of every five plans (covering 24 million patients) require members to resolve them through binding arbitration. And 10 percent of the 50 plans call for medical malpractice complaints to be settled that way, as well.
Now the California Research Bureau, the state equivalent of the US General Accounting Office, has issued a report condemning the arbitration process as unfair to patients.
For one thing, the report says, arbitration is expensive for most patients. For another, too many arbitration cases are summarily dismissed. That means the arbitrator has determined that the patient has presented too little evidence and that a hearing would be a waste of time.
Take Kaiser's summary judgment rate. From March 1999 to Jan. 5, 2001, 12 percent of Kaiser cases that went to arbitration were dismissed through summary judgment. By comparison, fewer than 1 percent of all civil complaints in state courts were dismissed that way in 2000.
What's more, California, like most states, has not established professional standards or licensing requirements for arbitrators. The American Bar Association, the American Arbitration Association, and the American Medical Association have attempted jointly to draft model procedures and standards for health care arbitration, but failed to reach agreement.
Direct-To-Consumer Ads: Do drug makers need a new Rx for educating patients?
Proponents of direct-to-consumer drug ads say they educate patients about medical conditions and treatments. But a recent study by researchers at the University of California found that those claims don't hold up.
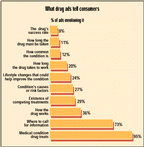
Richard L. Kravitz, director of the UC Davis Center for Health Services Research in Primary Care, and his co-authors (from UC Davis and UCLA) analyzed 320 ads promoting 101 medications. The ads appeared in 18 popular magazines between 1989 and 1998. On average, they scored only 3.2 on an 11-point scale measuring educational content. Most failed to provide information about a drug's success rate, how long it must be taken, or alternative treatments.
The majority, however, did mention the medical condition the drug is meant to treat (95 percent) and included a toll-free number to call for more information (73 percent).
The study was published in The Journal of Family Practice.
What drug ads tell consumers
Docket Watch: Ohio's high court limits parents' right to sue
Ruling in a pair of wrongful-life cases, the Ohio Supreme Court has denied plaintiffs the right to recoup damages for their children's injuries.
The first case involved a severely disabled girl who, along with her parents, sued her mother's obstetricians for damages stemming from congenital disabilities. The plaintiffs accused the doctors of withholding the results of prenatal tests that indicated the child would be born with defects. Had they known, the parents contended, they would have sought an abortion. The child, now 7, is seeking the cost of her medical and educational needs as well as damages for pain and suffering.
But Ohio doesn't recognize wrongful-life claimswhich seek to recover ordinary expenses associated with livingand the court found the case to be little more than a medical negligence action at its core. "We reject the suggestion . . . that [the child] suffered damage based on the fact of her being born rather than aborted," said Chief Justice Thomas Moyer, writing for the majority. "The only injury causally related to the [doctors'] breach of duty was the deprivation of the chance to make a fully informed decision whether to continue the pregnancy.
"That breach did not, in any way, cause [the child's] medical handicaps," Moyer said. Since the plaintiffs couldn't prove that it did, the high court upheld lower court decisions dismissing the suit.
The second case stemmed from the birth of an unplanned child following a faulty tubal banding. Born nearly a year after the procedure, the boy suffered from a heart defect and died at about 15 months of ageafter several open-heart surgeries and extended hospital stays. In an out-of-court settlement, the parents resolved their claims for pregnancy-related costs, the mother's pain and suffering, and the wages she lost during pregnancy and delivery.
But the issues of emotional distress and their son's medical bills went to court, and were denied at both the trial and appellate levels. The Ohio Supreme Court agreed, finding that the parents hadn't proven proximate cause. "Although a negligently performed sterilization is a proximate cause of a subsequent birth, it isn't a proximate cause of the birth defect," the court said. "Therefore, the negligent doctor can't be held liable for the costs associated with that defect."
Joan Rose. Practice Beat. Medical Economics 2001;5:16.





