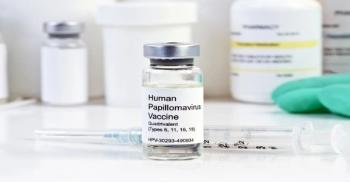
College-aged students still interested in HPV vaccine, especially when it’s free
College students who never received the HPV vaccine series are interested in getting the shot on campus, according to a new study. The study is a reminder, according to the authors, to physicians that it’s never too late to offer the series to young adults.
College students are still interested in getting vaccinated against human papillomavirus (HPV), even if they didn’t get the full vaccine in their childhood, according to a new study.
A. Scott LaJoie, PhD, MA, MSPH, a professor at the University of Louisville and co-author of the study,said the HPV vaccine is becoming more common among college students, so much so that it’s being considered as a part of their routine health care.
"This is great,” LaJoie said. “We should be promoting vaccination as a social norm. We want providers to engage their young patients in the decision to vaccinate or not. College students, in particular, are learning to evaluate evidence for themselves. Clinicians can facilitate this process by recommending information sources they know to be valid."
The
The survey showed that concerns over vaccine safety and the need for boosters did not have a negative impact, but that knowledge about the HPV-associated cancers the vaccine prevented didn’t have a positive impact on vaccination, either.
Researchers noted that parental influence availability of a free vaccine seemed to have the greatest influence on college-aged vaccination rates for HPV, with free vaccination alone doubled uptake in this population. The survey respondents also indicated a strong preference for a sexual partner to be vaccinated regardless of whether they themselves were vaccinated, according to the report.
Diane Harper, MD, MPH, MS, a clinical research expert in HPV and professor of medicine at the University of Michigan, co-authored the report and said the study shows that it’s not too late to vaccinate against HPV, even when patients reach their 20s.
“It’s important for college health professionals to offer college and graduate students the HPV vaccine as a step toward cervical cancer control,” she said. “For those women over 21 years, at the time of their cervical cancer screening, asking about HPV vaccination for future protection is prudent.”
By college age, some students have not been offered the vaccine or, for one reason another, did not receive the series. Harper pointed out that the college years offerthe time and opportunity to explore human relationships, which includes sexual exploration.
“Offering HPV vaccination to those not already vaccinated will offer some protection against this skin-to-skin spread of infection,” Harper said. “When offered to women in context of a spectrum of cervical cancer prevention opportunities, it provides an opportunity for women to understand that their sexual partners can be vaccinated as well, reducing even further the chances of their future HPV infection. Women prefer their male partners to be vaccinated, and men prefer their female partners to be vaccinated.”
Harper said she was surprised, however, to discover the level of influence parents still had on an individual’s health choices, even in college.
“It is surprising that at the college level, when young adults are encouraged to become independent rationale thinking adults, that parental influence about health would continue to be so strong,” she said.
Harper said it’s her hope that the study will promote continued cervical cancer screening for cancer control and prevention, and that the 20-and-older population will continue to seek out and be offered the HPV vaccine
LaJoie, added that it’s important for clinicians to remember that vaccinations don’t end in childhood.
“College-aged young adults want to be informed and engaged in the decision to vaccinate or not,” LaJoie said. “Clinicians should recognize their autonomy.”
LaJoie noted that some clinicians, especially in rural areas, are not recommending the HPV vaccine, and some young adults are reluctant to argue with their physicians or make their preferences known.
He added that the HPV vaccine has particular benefit for college students when it comes to the extended benefits of the HPV vaccine, like the prevention of genital warts in addition to cancers.
"The early 20s are a time when humans are at their peak fitness,” LaJoie said. “It is hard for a 20-year-old to imagine having cervical or penile cancer. HPV vaccines also protect them from genital warts. These unsightly and painful warts will definitely impact a person's potential love life. If preventing cancer isn't motivating enough, preventing genital warts should be.”
Newsletter
Stay informed and empowered with Medical Economics enewsletter, delivering expert insights, financial strategies, practice management tips and technology trends — tailored for today’s physicians.