Article
Assisted suicide? Pain control? Where's the line?
Physicians are evenly divided about assisted suicide, but most agree they need to treat pain better.
Assisted suicide? Pain control? Where's the line?
Physicians are evenly divided about assisted suicide, but most agree they need to treat pain better.
By Wayne Guglielmo
Senior Editor
Few if any ethical questions doctors face are more profoundand more profoundly disturbingthan the issue of physician-assisted suicide.
Proponents argue that a doctor's duty to alleviate suffering may justify the act, assuming the patient gives fully informed consent. Opponents counter that the Hippocratic oath expressly directs doctors to "do no harm." They point to religious and secular traditions that prohibit taking a human life, to the potential for abuse if assisted suicide is sanctioned, and to the inevitability of mistakes.
Legally, the debate has been equally intenseand the answer is clear cut. It's against the law in every state but Oregon. And the US Department of Justice, under Attorney General John Ashcroft, is challenging that state's law. (In late May, the DOJ appealed an earlier federal district court ruling that said the department lacked the authority to overturn the law.)
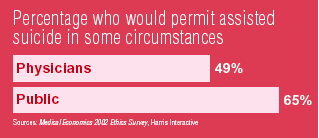
The physicians we surveyed are evenly divided on the issue49 percent say physician-assisted suicide should be permitted under some circumstances; 51 percent say No.
That split makes doctors far more conservative than the public-at-large. In a Harris Interactive poll conducted last year, 65 percent of the public indicated their support for assisted suicide.
But whatever the numbers say, the comments after the Yes or No answers make us wonder if actions follow words: Even doctors opposed to assisted suicide say making terminally ill patients comfortable, even at the risk of hastening death, is acceptable. "I'd have a hard time personally and ethically giving someone a lethal dose of medication," says David M. Whittiker, an FP in a five-member practice in Wichita Falls, TX. "But I wouldn't have a problem giving increasing doses of morphine until pain is relieved, knowing full well I'm subjecting the patient to some risk of death."
A distinction without a difference? Doctors like Whittiker hope not. He says he'd never want to "knowingly cause a patient's death, even for altruistic reasons." But other doctors admit it's a "gray area," a "matter of opinion" that could easily divide a well-intentioned jury.
Our survey also asked about the treatment of pain in a broader contextnot necessarily connected to end-of-life care. One respondent in four says that fear of outside forces like medical boards and prosecutors has caused them to alter treatment plans. Little surprise, then, that only about three in 10 say the medical profession is adequately dealing with patients' pain.
Few physicians help patients die
Although doctors as a group are split evenly on the question of physician-assisted suicide, there are some interesting differences when you look at the group by specialty. Support was highest among cardiologists (57 percent), and lowest among internists and pediatricians (42 percent). Whether this is because cardiologists see more people in worse shape than their colleagues or not is a matter for speculation.
Regionally, support is highest on the coasts. Physicians in the East are most likely to be in favor of assisted suicide (60 percent favor it). Only 43 percent of those in the Midwest do, and their Southern colleagues don't think much more highly of it, perhaps reflecting these regions' more conservative religious traditions.
Does practice follow theory? It appears to: Only 6 percentor fewer than 50of our respondents say they've ever helped a patient end his life. A frequently cited argument against the practice is religious conviction. "My God will not allow it," says one respondent. "I leave death to God," says another. But many doctors who cite their faith or the sacredness of life also echo David Whittiker, saying they've helped terminal patients with their pain, knowing that such treatment could cause them to die sooner. The comment made by family practitioner James P. McCann of Wabash, IN, is typical: "I would push pain medication and adjuvant therapy to get pain relief. It may possibly hasten death, but my goal in this life is patient comfort, not termination."
To some, this may seem like a contradiction, and perhaps it is. But to doctors whose religious convictions prohibit them from actually assisting in suicide, providing comfort at the end of life may be the most charitable and morally responsible course of action, despite the possible consequences.
Such justification is common. One in five of the doctors we surveyed says he's administered more pain medication than he considers optimal. Interestingly, cardiologiststhe doctors most likely favor assisted suicideare the least likely of the "adult" physicians to confess to doing so. Perhaps they just call it assisted suicide. Male physicians are also far more likely than their female colleagues to have administered more-than-optimal pain medication. Other doctors opposed to physician-assisted suicide say they've "withdrawn treatment" or "respected wishes not to use life support measures."
In its Code of Medical Ethics, the AMA encourages doctors to walk this narrow line between end-of-life care and assisted suicide: "Instead of participating in assisted suicide, physicians must aggressively respond to the needs of patients at the end of life. . . . Patients near the end of life must continue to receive emotional support, comfort care, adequate pain control, respect for patient autonomy, and good communication."
Some would say that, in leaving doctors to decide where comfort care ends and assisted suicide begins, the AMA and the American Geriatrics Society, among others, are treading a safe middle ground that offers confused physicians little help.
But some doctors appear to need less help with the matter than others. To emergency medicine specialist Amy F. Church of Williston Park, NY, for instance, palliative care is quite different from assisted suicide. She draws a distinction between a "lethal dose of medication administered under the guise of controlling pain" and a "dose sufficient to control the pain."
But Church doesn't discount the difficulty doctors face when they attempt to weigh their own duty "to do what's best overall" against a patient's right to determine "the situation of his own death," particularly if that patient is in severe pain. So for her, the question of physician-assisted suicide remains an open one. "I don't think I'll ever not be wrestling with it," she says.
Fear can drive pain treatment
On the broader issue of pain management, fear of official retaliation for aggressive treatment remains high among physicians, despite efforts in many states to relax policies on pain management. Some experts cite high-profile prosecutions as one reason for physicians' fear. Such prosecutionsespecially when they result from inadequate documentation rather than criminal intentremind physicians that they can still easily run afoul of the law.
That fear is operative comes through loud and clear in our survey: One out of every four respondents says he's changed a treatment plan because he fears litigation, disciplinary action, or prosecution. In effect, these doctors are acknowledging that they've put their own welfare above the welfare of their patients.
"That's distressing," says Estelle Rogers, executive director of Death with Dignity, a Washington, DC-based advocacy group. "In part because of the fear of regulation, doctors are willing to go back to the bad old days of undertreating pain, and that's bad news for patients."
But undertreating pain also carries legal risks, notes Barbara Coombs Lee, head of Compassion in Dying Federation, an Oregon-based patient advocacy group that helped win a lawsuit against a California internist who violated the state's elder-abuse law by undertreating pain.
In their comments, many respondents specifically mention Oxy-Contin, citing recent news stories and prosecutions as reasons they no longer prescribe the opioid, although they believe it has excellent pain-relieving properties. Others say fear of running afoul of the law as a reason they dispense a limited number of pain pills. Some, such as FP and dermatological surgeon T. Jeffrey Bernard of Shreveport, LA, say they often refer chronic pain patients on opioids to a pain management specialist rather than managing the case themselves.
"There's a general feeling among physicians in this area that the state medical board is looking over our shoulders," says Bernard. "Our ability to practice medicine is being questioned, and we're not able to treat patients as we think best."
Male physicians are almost twice as likely as female doctors to have changed a treatment plan because of possible reprisals. At first glance, the finding seems counterintuitive, given our cultural expectations of male courage. But in this instance, at least, empathy more than courage may be the guiding principle. Women physicians may simply be more willing to risk their own necks to ease their patients' suffering.
The bottom line on pain control? Only three doctors out of every 10 say that the medical profession has done an adequate job of treating pain. But there may be hope for the future: Younger doctors are more critical of the profession's performance than their older colleagues. "Ten years ago, doctors would have been more confident that their profession was treating pain adequately," says David Joranson, director of the Pain & Policy Studies Group at the University of Wisconsin's Comprehensive Cancer Center, in Madison. "But in the interim, there's been a tremendous effort to raise awareness about the inadequate management of pain."
Joranson and other experts also see reason for optimism as more enlightened pain programs and policies take hold. Says Joranson: "Ten years from now, we hope there will be a lot more confidence that pain is being treated well."
Wayne Guglielmo. Assisted suicide? Pain control? Where's the line?.
Medical Economics
2002;19:48.





